Pediatric mock codes, mirroring real emergencies, demonstrably improve survival rates in cardiopulmonary arrest. Resources like PALS guidelines and scenario PDFs are vital for effective simulation.
A. The Importance of Simulation in Pediatric Emergency Care
Simulation, utilizing realistic pediatric mock code scenarios – often available as PDFs – is paramount in preparing healthcare teams for critical events. These drills foster rapid decision-making and enhance teamwork without risking actual patient harm. Access to well-designed scenarios, mirroring conditions like respiratory distress or cardiac arrest, allows for repeated practice of PALS algorithms.
Effective simulation builds confidence and identifies skill gaps, leading to improved patient outcomes. Regularly reviewing and updating these pediatric emergency mock code scenarios, found in various PDF formats, ensures relevance and addresses evolving best practices. This proactive approach is crucial for optimal pediatric care.
B. Correlation Between Mock Codes and Improved Survival Rates
Research, including studies by Andreatta et al., demonstrates a significant correlation between regular mock code participation and improved pediatric cardiopulmonary arrest survival rates. Consistent practice with realistic pediatric emergency scenarios – frequently documented in accessible PDF formats – enhances team performance under pressure.
These simulations refine skills in areas like airway management, medication administration, and effective communication. Utilizing standardized mock code scenarios, often based on PALS guidelines and available as PDF resources, ensures consistent training. This translates to quicker response times and more effective interventions, ultimately boosting survival probabilities for critically ill pediatric patients.
C. Overview of Pediatric Cardiopulmonary Arrest Scenarios
Pediatric cardiopulmonary arrest scenarios frequently utilized in mock codes encompass a range of etiologies. Common simulations include respiratory failure due to asthma or foreign body aspiration, shock states (hypovolemic, septic), and various cardiac arrest rhythms – bradycardia, asystole, and ventricular fibrillation.
Detailed pediatric mock code scenarios, often available as downloadable PDF documents, provide structured frameworks for these drills. These resources outline patient presentations, vital signs, and expected interventions. Effective mock codes prepare teams to manage these critical events, emphasizing rapid assessment, appropriate interventions, and seamless teamwork, ultimately improving patient outcomes.

II. Core Components of a Pediatric Mock Code
Successful mock codes require defined team roles, essential equipment, and clear communication. Utilizing pediatric mock code scenarios, often in PDF format, ensures standardized training.
A. Team Roles and Responsibilities
Effective pediatric mock codes hinge on clearly defined roles. A designated leader directs the code, while a compressor provides continuous chest compressions, adhering to PALS guidelines found in scenario PDFs. Another team member manages the airway, ensuring proper intubation or ventilation. Medication administration falls to a dedicated individual, verifying age-appropriate dosages.
A scribe meticulously documents all interventions and times, crucial for debriefing. Runners swiftly retrieve necessary equipment and medications; Observing and evaluating the team’s performance is vital, often utilizing checklists derived from pediatric mock code scenarios. Each role’s responsibility must be understood to foster seamless teamwork and optimize patient outcomes during simulated emergencies.
B. Essential Equipment and Medications
Successful pediatric mock codes demand readily available, functional equipment. This includes age-appropriate bag-valve-masks (BVMs), laryngoscope blades, endotracheal tubes, and suction devices. Monitoring tools – pulse oximeters, cardiac monitors, and capnography – are crucial for assessing patient status. Access to defibrillators with pediatric pads is non-negotiable.
Essential medications, guided by pediatric mock code scenarios and PDFs, encompass epinephrine, adenosine, and fluids. Dosage charts reflecting weight-based calculations must be visible. Having a Broselow tape simplifies medication and equipment sizing. Regular inventory checks ensure all items are present and within expiration dates, guaranteeing a realistic and effective simulation.
C. Communication Protocols During a Code
Clear and concise communication is paramount during pediatric mock codes. A designated “code leader” directs the team, assigning tasks and ensuring a systematic approach. Utilizing a closed-loop communication system – stating the order, repeating the order, and confirming understanding – minimizes errors. Standardized terminology, aligned with PALS guidelines and pediatric mock code scenarios found in PDFs, is essential.
Briefings and debriefings should emphasize effective communication strategies. Regularly practicing SBAR (Situation, Background, Assessment, Recommendation) enhances information transfer. Maintaining a calm and respectful tone, even under pressure, fosters teamwork and optimal patient care during simulated emergencies.
III. Common Pediatric Mock Code Scenarios
Frequent simulations involve respiratory distress, shock (hypovolemic, septic), and cardiac arrest. Accessing detailed pediatric mock code scenarios in PDF format aids realistic training.
A. Respiratory Distress & Failure
Simulating respiratory emergencies is crucial, encompassing asthma exacerbations, croup, epiglottitis, and foreign body aspirations. Utilizing pediatric mock code scenarios, often available as PDF downloads, allows teams to practice rapid assessment and intervention. These scenarios should challenge participants to differentiate between varying degrees of distress, from mild wheezing to complete airway obstruction.
Effective drills necessitate realistic presentations, including appropriate vital signs and clinical findings. Emphasis should be placed on bag-valve-mask ventilation, oxygen administration, and potential intubation. Access to detailed PDF resources provides standardized cases, ensuring consistent training and skill development across the healthcare team, ultimately improving patient outcomes.
B. Shock (Hypovolemic, Septic, Cardiogenic)
Pediatric shock simulations – hypovolemic from dehydration, septic from infection, or cardiogenic post-surgery – demand rapid recognition and intervention. Comprehensive pediatric mock code scenarios, frequently found as downloadable PDF guides, are essential for training. These scenarios should focus on fluid resuscitation, vasopressor administration, and identifying the underlying cause of shock.
Realistic simulations require accurate vital sign manipulation and clinical presentations. Teams must practice differentiating shock types and implementing appropriate treatment protocols. Utilizing standardized PDF resources ensures consistent training, emphasizing age-specific dosages and interventions. Effective drills improve the team’s ability to manage critically ill children experiencing shock.
C. Cardiac Arrest (Bradycardia, Asystole, PEA, VF/VT)
Pediatric cardiac arrest simulations, encompassing bradycardia, asystole, pulseless electrical activity (PEA), and ventricular fibrillation/pulseless V-tach, necessitate swift and coordinated responses. Detailed pediatric mock code scenarios, often available as PDF downloads, provide structured training opportunities. These scenarios should emphasize early CPR, defibrillation (when indicated), and adherence to PALS guidelines.
Effective drills require realistic rhythm interpretation and medication administration. Teams must practice escalating interventions based on the arrest rhythm and response. Utilizing standardized PDF resources ensures consistent training, focusing on age-specific dosages and the importance of high-quality chest compressions. Mastering these skills improves outcomes in genuine pediatric cardiac arrest events.
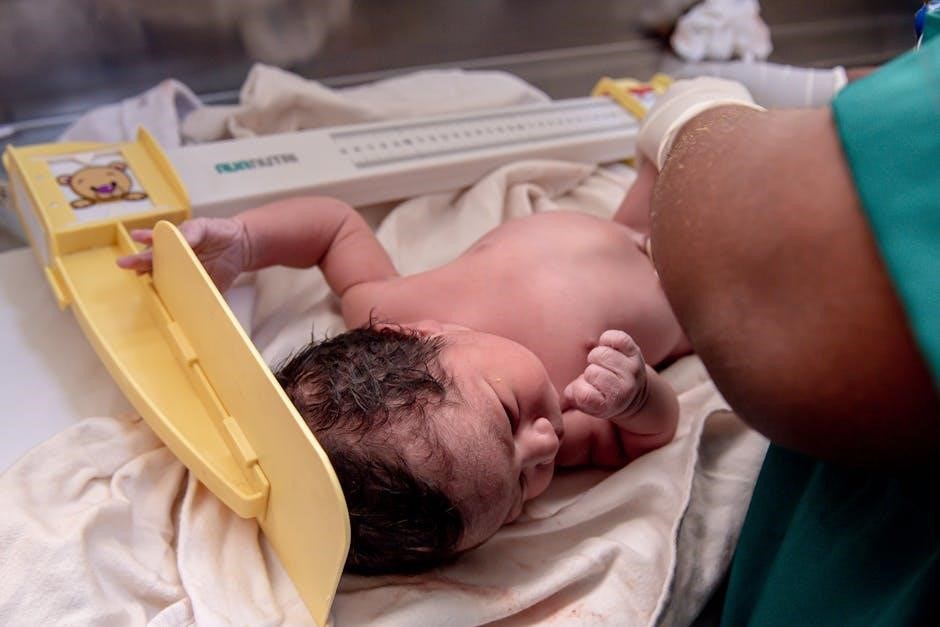
IV. Specific Scenario Breakdown: Respiratory Distress
Respiratory distress simulations, detailed in pediatric mock code scenarios PDFs, cover asthma, croup, and foreign body aspiration, demanding rapid assessment and intervention.
A. Asthma Exacerbation Simulation
Asthma exacerbation simulations, frequently found within comprehensive pediatric mock code scenarios PDFs, necessitate a focused approach. The scenario should begin with escalating respiratory distress – wheezing, retractions, and increasing work of breathing. Participants must accurately assess the child’s condition, utilizing pulse oximetry and auscultation.
Effective management involves prompt oxygen administration, nebulized bronchodilators (albuterol), and potentially systemic corticosteroids. The simulation should challenge teams to recognize signs of impending respiratory failure and initiate appropriate interventions, including considering non-invasive ventilation or intubation. PDF resources often detail escalating treatment algorithms and expected physiological responses, enhancing realism and learning.
B. Croup & Epiglottitis Mock Code
Croup and epiglottitis mock codes, detailed in many pediatric mock code scenarios PDFs, demand rapid assessment and decisive action. Simulations should present a child with stridor, drooling, and difficulty breathing – differentiating between the two is crucial. Epiglottitis requires heightened suspicion for airway obstruction.
Initial management focuses on airway maintenance, often involving positioning and supplemental oxygen. Racemic epinephrine nebulization is key for croup, while epiglottitis necessitates careful intubation preparation. PDF resources emphasize the importance of avoiding airway manipulation in epiglottitis until a controlled airway is secured. Teams must demonstrate proficiency in recognizing escalating airway compromise and implementing appropriate interventions swiftly.
C. Foreign Body Aspiration Scenario
Foreign body aspiration (FBA) mock codes, frequently found within pediatric mock code scenarios PDFs, require immediate recognition and intervention. Simulations should depict a child exhibiting sudden onset of coughing, wheezing, or respiratory distress, potentially progressing to cyanosis. Age-appropriate techniques are paramount; back blows and chest thrusts for infants, and abdominal thrusts for older children.
PDF resources highlight the importance of avoiding blind finger sweeps. Successful scenarios involve prompt airway visualization and removal of the obstructing object. Teams must demonstrate proficiency in utilizing bag-valve-mask ventilation if respiratory failure occurs, preparing for potential endotracheal intubation. Effective communication and coordinated teamwork are vital for a positive outcome in these time-critical events.
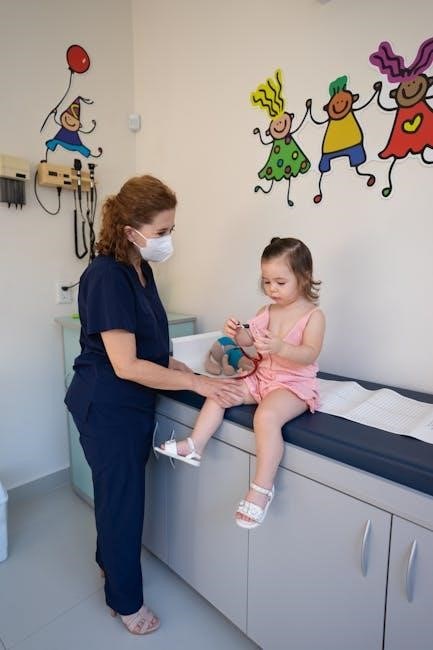
V. Specific Scenario Breakdown: Shock
Shock simulations, detailed in pediatric mock code scenarios PDFs, necessitate rapid assessment and intervention for hypovolemic, septic, and cardiogenic etiologies.
A. Dehydrated Infant with Hypovolemic Shock
Hypovolemic shock in infants, often stemming from dehydration – perhaps due to gastroenteritis or inadequate fluid intake – demands swift recognition and intervention. Pediatric mock code scenarios PDFs frequently feature this presentation, emphasizing initial assessment of perfusion: capillary refill, heart rate, and respiratory effort.
Simulations should focus on appropriate fluid resuscitation utilizing age-specific boluses, monitoring response, and considering underlying causes. Failure to provide high-flow oxygen, a common error highlighted in EMT scenarios, must be addressed. Participants should practice differentiating between mild, moderate, and severe dehydration, guiding appropriate treatment strategies. Accurate documentation of fluid administration and patient response is crucial for effective management.
B. Pediatric Sepsis Simulation
Pediatric sepsis simulations, readily available in mock code scenarios PDFs, necessitate rapid identification of systemic inflammatory response syndrome (SIRS) criteria and potential sources of infection. Emphasis should be placed on early antibiotic administration, ideally within the first hour, following appropriate cultures.
These scenarios should challenge participants to differentiate between septic shock and other causes of shock, focusing on vital sign trends and clinical presentation. Effective fluid resuscitation, vasopressor support if needed, and meticulous monitoring of organ perfusion are key. Recognizing thrombotic complications, more prevalent in pediatric patients with underlying conditions, is also vital during simulation exercises.
C. Cardiogenic Shock Post-Cardiac Surgery
Cardiogenic shock simulations post-cardiac surgery, often detailed in mock code scenarios PDFs, require a focused assessment of cardiac function. Participants must interpret hemodynamic parameters – flow, pressure head, and RPM – as seen in LVAD patients (e.g., flow 2.4 l/min, pressure 71.6 mmHg).
Scenarios should emphasize inotropic support, afterload reduction, and volume management to optimize cardiac output. Recognizing potential complications like arrhythmias or mechanical device malfunction is crucial. Effective communication between the surgical team and critical care providers is paramount. Understanding congenital heart disease and its impact on post-operative recovery is also essential.

VI. Specific Scenario Breakdown: Cardiac Arrest
Cardiac arrest simulations, often found in pediatric mock code scenarios PDFs, cover bradycardia, asystole, PEA, and VF/VT, demanding rapid PALS algorithm application.
A. Bradycardia with Compromised Perfusion
Bradycardia scenarios, detailed within pediatric mock code scenarios PDFs, necessitate swift assessment of perfusion status. Participants must demonstrate proficiency in recognizing signs of poor perfusion – altered mental status, cool extremities, and diminished pulses – alongside appropriate interventions.
Simulations should challenge teams to apply PALS guidelines, including oxygenation, ventilation, and potentially, pharmacological interventions like atropine; Emphasis should be placed on continuous cardiac monitoring and timely escalation to chest compressions if perfusion remains compromised. Effective communication and teamwork are paramount in managing this critical situation, mirroring real-world pediatric emergencies.
B. Asystole Following Prolonged Arrest
Pediatric mock code scenarios PDFs often feature asystole cases following extended cardiac arrest, demanding a systematic approach. Participants must demonstrate proficiency in high-quality CPR, ensuring adequate rate and depth of compressions, alongside coordinated ventilation.
Simulations should emphasize the importance of epinephrine administration, as per PALS guidelines, and the need for continuous rhythm analysis. Teams must effectively communicate and rotate compressor roles to minimize fatigue. Recognizing the futility of prolonged resuscitation without response is also crucial, prompting discussions about end-of-life care considerations.
C. Ventricular Fibrillation/Pulseless V-Tach
Pediatric mock code scenarios PDFs frequently include ventricular fibrillation (VF) or pulseless ventricular tachycardia (VT) cases, requiring immediate defibrillation. Simulations must assess the team’s speed and accuracy in recognizing these rhythms and delivering appropriate energy levels, adjusted for pediatric weight.
Effective chest compressions during charging and immediately after shock delivery are paramount, alongside epinephrine administration. Post-shock rhythm analysis is critical; continued VF/VT necessitates repeat shocks. Teams should demonstrate understanding of the PALS algorithm and clear communication throughout the resuscitation effort, emphasizing a coordinated response.

VII. Utilizing Pediatric Advanced Life Support (PALS) Guidelines
PALS algorithms are central to pediatric mock codes, with PDF resources aiding skill evaluation. Age-specific dosages and interventions must be consistently applied during simulations.
A. PALS Algorithm Integration into Mock Codes
Integrating Pediatric Advanced Life Support (PALS) algorithms into mock codes is paramount for effective training. Utilizing readily available pediatric emergency scenario PDFs allows teams to practice systematic responses to critical events. These scenarios should directly mirror PALS pathways for bradycardia, respiratory failure, and shock.
Successful implementation requires participants to verbalize each step of the algorithm, ensuring a shared mental model. Mock codes provide a safe environment to identify gaps in knowledge and refine skills. Regularly updating scenarios, based on current PALS guidelines and downloadable resources, maintains relevance and optimizes preparedness. Emphasis should be placed on accurate application of age-specific interventions.
B. Skills Checklist Evaluation During Simulations
Employing a detailed skills checklist during pediatric mock codes, often found within comprehensive pediatric emergency PDF resources, is crucial for objective assessment. Checklists should evaluate core competencies like CPR proficiency, medication administration accuracy (age-specific dosages!), and effective airway management techniques.
Observers utilize the checklist to document performance, identifying strengths and areas needing improvement. This structured evaluation extends beyond technical skills to encompass teamwork, communication, and leadership. Post-simulation debriefing should directly reference checklist findings, fostering constructive feedback. Utilizing standardized checklists ensures consistent evaluation across all mock code scenarios and participants.
C. Emphasis on Age-Specific Dosages and Interventions
Pediatric emergencies demand precise, age-specific interventions – a critical focus within mock code scenarios and detailed in PDF guides like PALS materials. Medication dosages, airway equipment sizes, and even chest compression depths vary dramatically based on a child’s weight and developmental stage.
Mock codes must actively challenge participants to calculate and administer correct dosages, reinforcing the dangers of adult-based protocols. Simulations should incorporate scenarios requiring nuanced interventions tailored to infants, toddlers, and older children. Regularly reviewing age-specific algorithms, often included in scenario PDFs, is paramount for optimal patient outcomes.
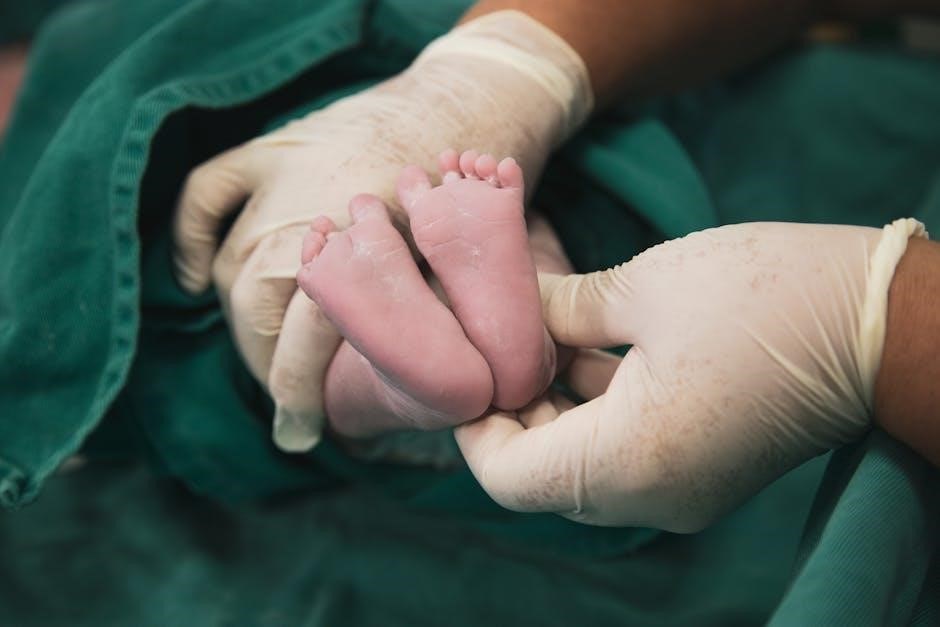
VIII. Advanced Considerations in Pediatric Mock Codes
Mock code scenarios, often found in PDF format, should integrate complex cases like congenital heart disease, LVAD considerations, and thrombotic risks for realism.
A. Congenital Heart Disease & LVAD Considerations
Pediatric mock codes involving congenital heart disease require nuanced understanding of altered physiology and potential complications. Scenarios should incorporate patients with failing Fontan circulations or single-ventricle physiology. LVAD (Left Ventricular Assist Device) considerations are crucial; PDF resources detailing appropriate flow rates, pressure monitoring (e.g., 2.4 l/min flow, 71.7 mmHg pressure head), and troubleshooting alarms are essential.
Simulations must address potential issues like pump thrombosis, device malfunction, and the impact of altered hemodynamics on resuscitation efforts. Teams should practice managing anticoagulation, recognizing signs of device failure, and coordinating with cardiac specialists. Realistic scenarios enhance preparedness for these complex pediatric emergencies.
B. Thrombotic Complications in Pediatric Patients
Pediatric mock codes must address the heightened risk of thrombotic events, particularly in patients with congenital heart disease or central venous catheters. PDF resources outlining age-specific dosing of anticoagulants and thrombolytics are invaluable. Scenarios should simulate presentations like acute limb ischemia, stroke, or pulmonary embolism, demanding rapid recognition and intervention.
Teams should practice assessing for signs of thrombosis, initiating appropriate diagnostic studies, and implementing treatment protocols. Consideration should be given to the challenges of anticoagulation reversal and the potential for bleeding complications. Realistic simulations, guided by detailed PDF checklists, improve preparedness for these critical situations.
C. Addressing Chronic Hypoxia in Simulations
Pediatric mock codes should incorporate scenarios involving patients with pre-existing chronic hypoxia, such as those with cystic fibrosis or severe asthma. PDF resources detailing baseline oxygen saturation goals and appropriate escalation strategies are crucial. Simulations must challenge teams to differentiate acute decompensation from chronic baseline, avoiding over-correction.

Scenarios should emphasize the importance of careful respiratory assessments, recognizing signs of impending respiratory failure, and initiating non-invasive or invasive ventilation. Teams should practice managing the complexities of long-term oxygen therapy and anticipating potential complications. Utilizing detailed PDF checklists ensures comprehensive evaluation.
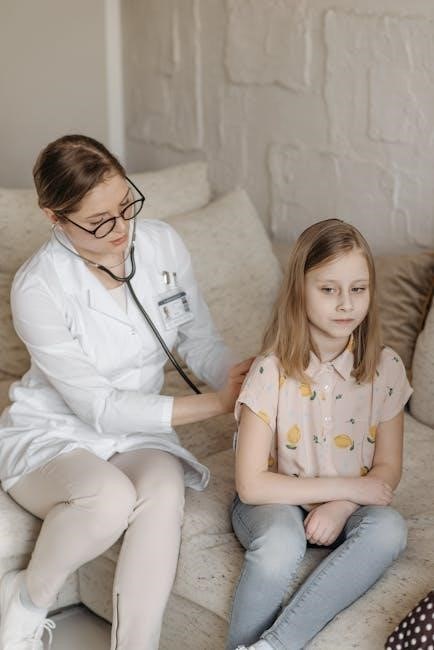
IX. Debriefing and Continuous Improvement
Structured debriefings, utilizing PDF checklists, identify areas for improvement after each mock code. This fosters a culture of learning and enhances pediatric care.
A. Structured Debriefing Techniques
Effective debriefing post-mock code is crucial for learning and skill refinement. Utilizing a standardized approach, perhaps guided by a PDF checklist derived from PALS guidelines, ensures comprehensive review. Begin with participant self-reflection – what went well, what could be improved? Then, focus on the scenario itself, analyzing team dynamics, communication effectiveness, and adherence to protocols.
Encourage open, non-judgmental discussion. Explore critical actions, decision-making processes, and any deviations from established algorithms. Review the use of essential equipment and medications. Finally, translate insights into actionable steps for future training and improved pediatric emergency response. A well-structured debrief maximizes the educational value of each simulation.
B. Identifying Areas for Improvement
Post-mock code analysis, informed by PALS guidelines and potentially utilizing scenario PDFs for comparison, reveals critical improvement areas. Common deficiencies include communication breakdowns, delayed recognition of deteriorating conditions, or incorrect medication dosages. Assess adherence to established algorithms – were steps followed sequentially and accurately?
Evaluate team role clarity and individual performance. Identify gaps in knowledge regarding age-specific interventions or management of complex cases like congenital heart disease. Document these findings systematically. Prioritize areas needing focused retraining, potentially incorporating additional simulations targeting specific skills. Continuous improvement relies on honest self-assessment and targeted interventions.
C. Documentation and Follow-Up Actions
Thorough documentation of each mock code, referencing utilized pediatric scenarios – potentially from PDF resources – is crucial. Record participant roles, interventions performed, identified errors, and debriefing feedback. This data informs targeted retraining and competency assessments.
Follow-up actions should include scheduled refresher sessions addressing identified weaknesses, particularly regarding PALS algorithms and age-specific dosages. Track completion of these actions and reassess competency through subsequent simulations. Ensure documentation is readily accessible for quality improvement initiatives and regulatory compliance. Consistent follow-up reinforces learning and promotes sustained skill enhancement.

X. Resources for Pediatric Mock Code Development
Access diverse pediatric emergency scenarios, including downloadable PDF versions, via online databases and PALS course materials to enhance simulation realism.
A. Online Databases of Pediatric Emergency Scenarios
Numerous online platforms offer a wealth of pediatric emergency scenarios, frequently available as downloadable PDF documents. These resources are invaluable for developing realistic mock codes, covering a spectrum of conditions from respiratory distress to cardiac arrest. Searching for “pediatric mock code scenarios PDF” yields results from hospital systems and educational institutions.
These databases often categorize scenarios by age group and acuity, facilitating targeted training. Many include detailed patient histories, vital signs, and expected interventions. Utilizing these pre-built scenarios saves time and ensures comprehensive coverage of essential pediatric emergency skills. Remember to verify the source and date of the PDF to ensure alignment with current PALS guidelines.
B. PALS Course Materials and Updates
Pediatric Advanced Life Support (PALS) course materials represent a cornerstone for mock code development. The official PALS provider offers case-based scenarios, often adaptable for simulation exercises, and frequently available as supplementary PDF resources for participants. Regularly reviewing PALS updates is crucial, as algorithms and recommendations evolve.
These materials provide a standardized framework for approaching pediatric emergencies, ensuring consistency in training. While not always directly presented as complete “mock code scenarios PDFs”, they contain the foundational elements – patient presentations, algorithms, and skill checklists – necessary to construct robust simulations. Supplementing PALS content with additional scenarios enhances realism and skill retention.
C. Accessing Pediatric Mock Code PDFs
Locating dedicated “pediatric mock code scenarios PDFs” requires targeted searching; Many hospital systems and educational institutions develop internal resources, sometimes shared through professional networks or conferences. Online databases, while not always comprehensive, can yield valuable examples. Searching for “PALS mock codes PDF” or “pediatric emergency simulation scenarios” broadens the scope.
However, be critical of source reliability. Ensure scenarios align with current PALS guidelines and reflect best practices. Consider adapting existing materials rather than relying solely on pre-made PDFs. Creating custom scenarios tailored to your team’s needs and local resources often proves more effective for targeted skill development and realistic training.



